have hospitals really been overloaded?
separating truth from TV soap opera (especially in the minds of the doctors)
one of the more persistent and sensationalist claims made around covid has been that it has “overwhelmed hospitals” and that we all must change our lives and surrender our livelihoods to “protect them.” this was the literal underpinning of the initial policy response of “2 weeks to flatten the curve.” we, it was alleged, needed to all stay home and distance for 2 weeks to stop the spread and keep covid from overwhelming hospitals.
the evidence that this never worked, could not have worked, and that all the standing evidence based guidelines for pandemics for the last 100 years said it wouldn’t is legion and overwhelming. i won’t foray further into that here.
but the other key question is this: did the hospitals really need protecting?
just how severe was and is this issue purportedly requiring such dramatic ends to mitigate?
it turns out, not very severe at all. in fact, in nearly all places and nearly all times, it was very much the opposite.
let’s start with a few salients:
hospitals are dramatic places. there’s lots going on and crisis is a daily occurrence. there is a reason there are so many soap operas and TV dramas set there. (and it’s not, tik tok notwithstanding, that hospital staff are such wonderful dancers)
hospitals are also businesses. they establish and maintain capacity based on demand. they seek to be full and to be utilized. 80-90% of beds being full is absolutely normal. in peak season, so is 95% or 100%. this is what they aim for.
this is even more true of ICU where keeping a staffed bed empty is very expensive (and only staffed beds are counted). by law, every US hospital must be able to increase ICU capacity by 25% (to 125%) on little or no notice. many can flex more like 50% and some even more. “100% ICU use” is not a crisis nor a sign that beds are not available.
the media loves crises, dramatic stories, and scaring the bejesus out of the citizenry. it’s good for readership. it’s even better if you can use it to vilify people you don’t like.
there is always, somewhere, a doctor having a bad day and looking to vent or devolving into hysterics because they are just not cut out for hospital life. it’s a hard, hectic place, and like wall st, has a high washout rate. people get attracted to the glamor, the money, the status, and the excitement, but many cannot hack the stress. that’s just the way it is. always was.
it’s not hard to see how these facts create a confluence conducive to histrionic reporting, especially given the sort of things that are selectively amplified on social media. it’s quite literally a perennial story. we just didn’t used to freak out and cancel the world over it. remember the hospital tent crisis of 2018? (thought not)
but what makes this whole affair so truly lamentable is that unlike most of covid there is LOTS of good data, available in near real time, and for free. yet almost no one is checking facts and we’re still fighting over this as though there is a real issue here.
there isn’t. it’s 99% hallucination and fabrication and always was.
the repetition of these news stories and claims creates a sense that it must be true because you’ve heard it so many times and the sheer volume of it seems to demand your belief in its veracity. but that’s exactly how propaganda works.
repetition becomes reality and fearsome, emotional appeals and gaslighting prevent those who doubt it from speaking up for fear of being called evil and gang tackled by the winged monkeys of cancel culture.
but what’s fascinating is just how EASY it is to dismantle each of these claims.
i have yet to see one really stand up. the US hospital system is, in fact, extremely robust, especially once you get away from a few perennial basket cases like NYC that are simply grossly under-capacitied and have been for decades.
some have been telling the truth of this narrative. but let’s see what happens when they do.
first, you always get the serious kooks and trolls who are either pretending to be doctors or have seriously lost the plot.
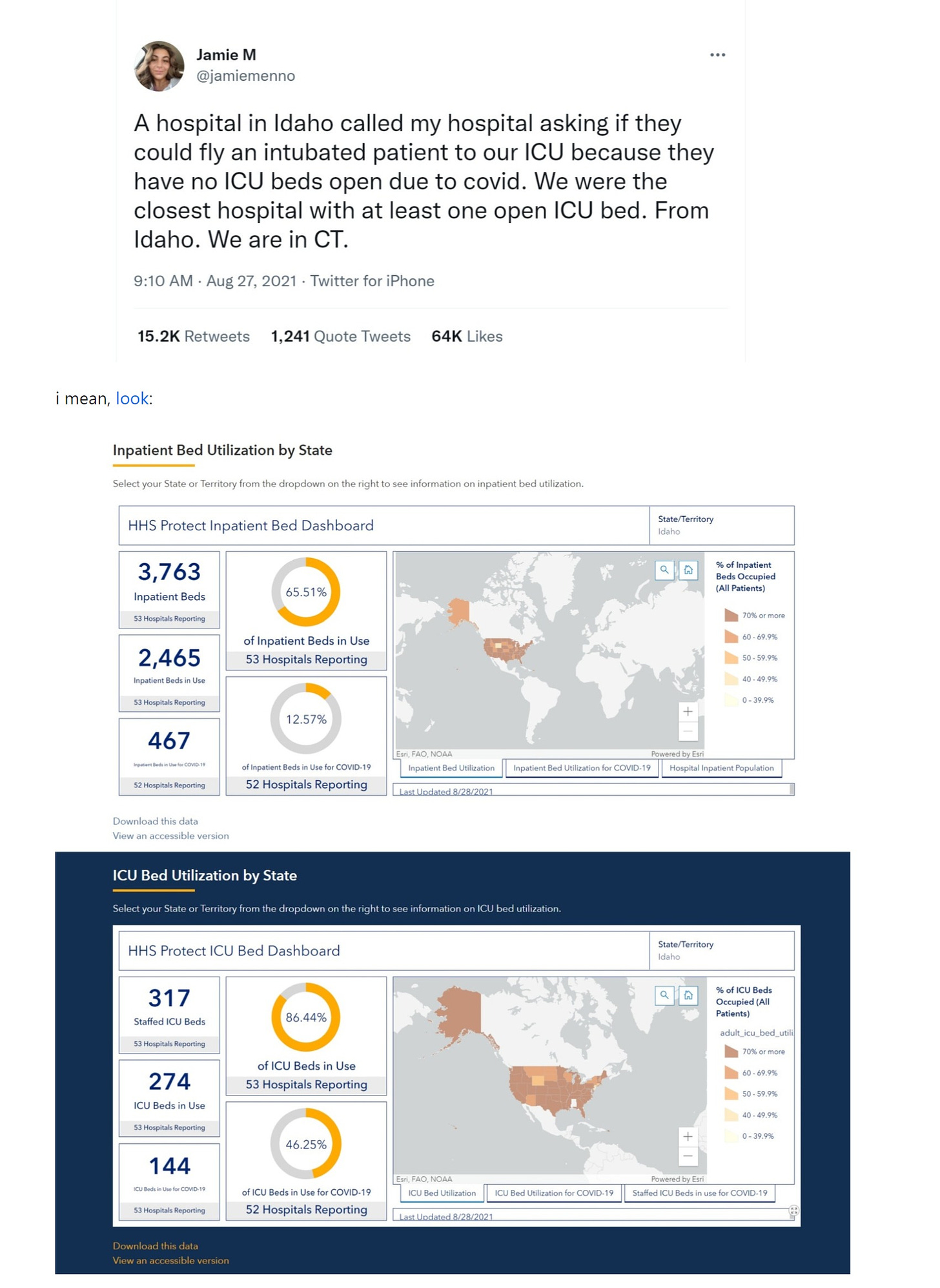
it tends to look like this:
is there seriously any sane human that thinks there was ever a time of no ICU beds within 1000 miles in the US? there has never even been a single state where this has happened. it’s a completely made up story told for dramatic effect and dishonest image manipulation. it’s a weaponized media trope designed to terrify. even a kitten can see this:
so let’s dispense with that. clearly, there are a lot of people who are, for whatever reason, telling a lot of lies about what’s going on.
and you can always check it HERE using the HHS tools. (bookmark it. this is a crowd sourced propaganda campaign, so we need crowd sourced debunking)
but what about the more credible folks, the “experts” and people we really know to be doctors? here we have megan ranney, blue check and actual doctor at brown university emergency medicine.
alas, like many others from the gato alma mater (like jha over at the school of public health) meghan seems to struggle with reality and sense of proportion. her twitter feed speaks for itself. but how about her facts? has this hospital in which she works truly been overwhelmed?
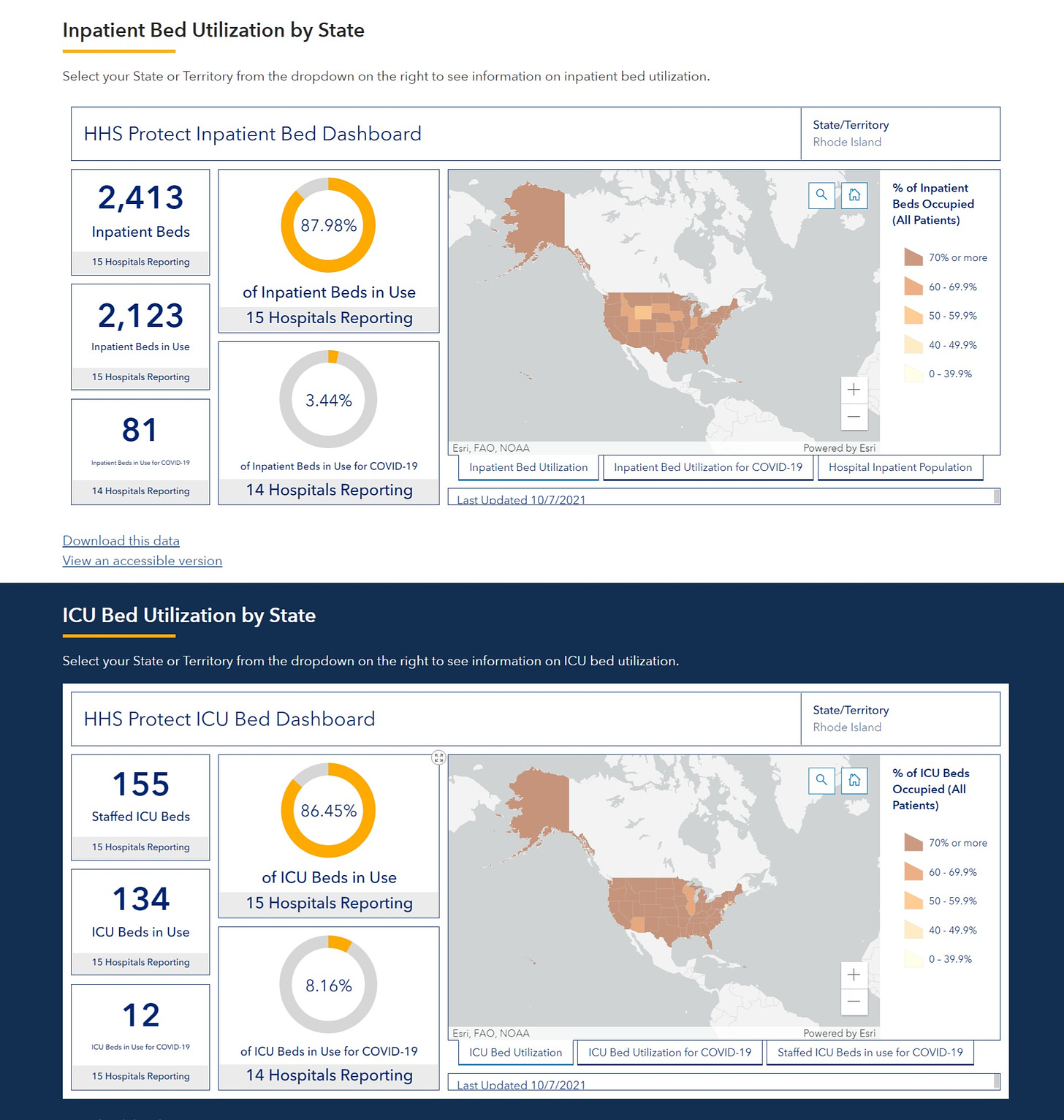
it sure seems implausible that it is at the moment. rhode island looks pretty normal and to the extent that hospitals are full, it sure does not seem to be from covid. 3% of beds and 8% of ICU does not seem like much of an overwhelming crisis.
but perhaps this is unfair as this is a low season and they were, indeed, overwhelmed in the past year.
these hospitals have investors and they report their figures publicly. so the data is all there. (perhaps ms ranney may be forgiven for not knowing this as doctors are notoriously poor investors)
to assess this, i turn to gatopal™ stinson norwood who took a bit of a run down finance’s memory lane and turned up some quite telling information.


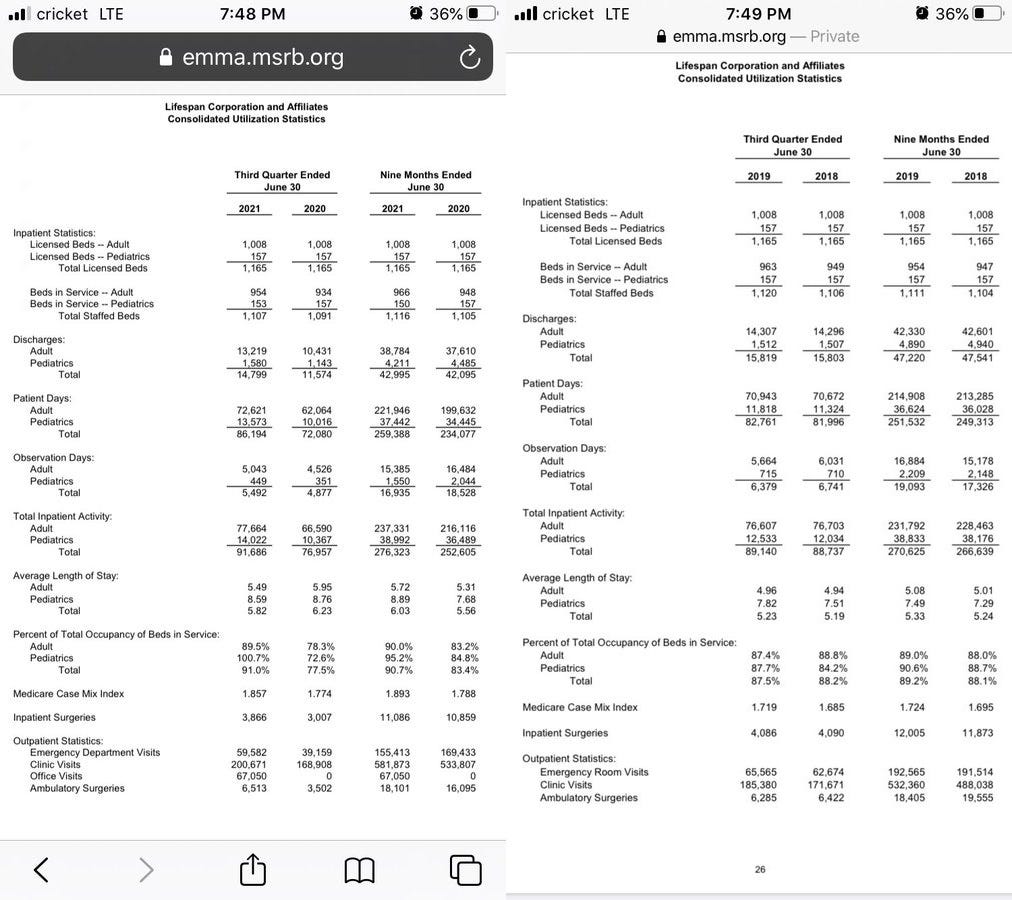
as meghan works in the ER, this seems a good place to start. and so he does and in doing so, helps to establish a pattern we see all over the US:
yes, hospitalization use is up a fair bit from 2020 to 2021, but this is NOT because use is surging to unusual levels.
it’s because 2020 was so incredibly low that half the hospitals in the US nearly went out of business and probably would have if they had not been propped up by a torrential flood of federal CARES money.
to make this clear, i graphed it:
this is the world where meghan works. unless someone remembers something i do not, 2019 was a pretty normal and unobjectionable year. 2020 was 40% lower in in the ER. that’s “going out of business” quiet.
2021 was still 9% below 2019. (and 5% below 2018) so, again, we’re nowhere near “overwhelmed.” we’re “a bit slow.”
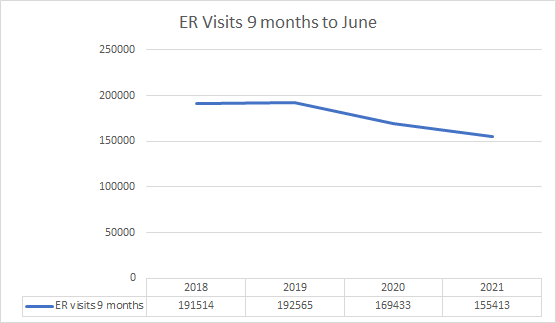
but perhaps this is still unfair because june is low season for covid. so let’s look at the 9 months ending june so it includes Q4 of last year and Q1 of this. those ARE peak covid seasons in RI.
we see the same thing except that 2021 is below even 2020. this 9 mo period was 19% lower than the same period of 2019 and, amazingly, 8% below last year.
this is not “overwhelmed.” this is “quietest in decades.”
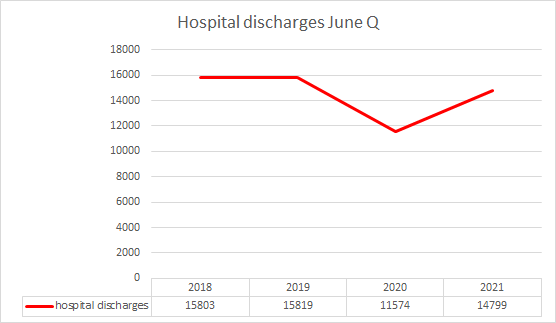
the same pattern can be seen in overall hospital discharges.
so to what do we attribute this powerful sense of stress?
how are we to explain all these doctors having such melt-downs and describing such dire conditions in their hospitals?
because damn near every single hospital system is the US looks like this. you can read 100 debunkings of these seemingly endless claims HERE as collected by gatopal™ @elonbachman, a literal lepidopterist of hospital scare stories.
by any historical standard, hospital traffic is low, not high.
i know a fair few doctors in hospitals, and more than a couple ARE freaking out right now. they do feel overwhelmed. they are not all propogandists and partisan hacks. i believe many of them to sincerely feel this.
and i think they reason is simple: habituation.
they got used to hospitals being dead quiet. they had basically a whole year of really low workflow. everyone was afraid, no one came, even to ER’s.
but ER traffic in Q2 of 2021 is up 50% from a year ago at the ER of dr ranney. it’s still low compared to a typical year, but that must seem MASSIVE after the lazy tik tok dancing days of the summer of 2020.
when you get used to “way below normal” a return to “almost normal” might well feel like crisis.
people all over the US are having similar experiences as they go back to in person work and try to start moving at the rapid pace they used to. people are quitting jobs and having breakdowns in droves. they got used to working 5 hours a day in their jammies. a return to normal is a big step up in workload.
why would doctors be any different?
(and let’s face it, doctors are affected by media and zeitgeist just like the rest of us. relentless stories about how hospitals are overloaded makes doctors feel like it’s real just like endless stories about shark attacks make everyone see fins in the water.)
it’s not the systems that are overwhelmed, it’s the emotions of the doctors after a year of low hospital use and it is not we whose perspective must shift to match theirs but rather theirs that must shift to rejoin reality.
this is the speed at which “hospital” has always been played. they used to handle it without any undue fuss because that’s how medicine works and that’s how good and how tough doctors have to be. no one said it was easy.
so perhaps the honest prescription for the doctors is “rub a little dirt on it and get back in there” because this IS normal, and it’s time to normalize that…








I am a physician in a private practice in FL next door to an urgent care. Whenever I walk over there to get my mail, the lobby is empty and the nurses are texting on their phones. I even asked them over the summer how the delta was affecting things. They giggled and said it was the "older people/worried well with sniffles who had been vaxxed who were testing positive". The populace is still scared to go there. It worries me that they will shut down due to going bankrupt. The hospitals have a financial incentive to continue to "cry covid" and get the sickest intubated people shuffled thru, there is a government bounty tied to the +PCR and until that is rescinded--I can dream right?--things will never be normal. I read a recent article that stated 20% of all healthcare workers over the past 18 months have been reshuffled/retired/quit/started new jobs and this churn is causing massive stress to those left behind in the trenches. The doctors and nurses are in hysterics over having to mask/gown all day long for 18 months--every patient is a bag of virus!--my question is why continue to mask if you're not sick/ symptoms? STOP THE PERFORMANCE THEATER. I no longer wear a mask in my office nor do I "make" anybody wear it either. I wore the same dirty mask for 3 weeks at a time last year when I couldn't buy any for my clinic and I literally had 5 masks left, and after my 3rd eyelid chalazion from steam blowing up to my eyes and the end of the "Health Emergency" in FL, I stopped in May 2021. Not one person has been infected from being in my office, nor myself, in 18 months of this BS and I'm a doctor taking care of elderly and immunosuppressed patients. One at a time, each one us must push back and live as normally as possible.
I am somewhat dismayed that you have ONLY 10K subscribers. Your work deserves 10M or 100M subscribers!